Anyway, eventually it hit 7:30am and the local crew arrived so it was time to bring some serious professionalism to the table – so we won them over with egg and bacon sandwiches for a few minutes before cracking on with the educational discussion.
For this session the local GP’s requested a debrief and over view of a recent case.
The GP’s talked us through the case. A local man was wheeled into the practice by his mate, with a GCS of 6, in severe respiratory distress.
This gentleman lived in local community housing, with a history of COPD, schizophrenia and subsequent poor self-care. Despite living in Geeveston for the last 8 years this man hadn’t previously attended the local GP practice, so they didn’t have medical history available.
Upon receiving the patient, they called AT for assistance and retrieval – which was rapidly escalated to the chopper.
The patient was semi-conscious, initially non-combative, no audible breath sounds on auscultation and was peripherally shut down. They provided some ventilatory assistance via a BVM then swapped to back to back nebulisers with salbutamol and ipratropium. They also commenced an adrenaline infusion – 1mg in 1Litre over 1 hour. They were very excited about this as they were taught this infusion at the previous EMET session which incidentally was the day before this patient arrived.
The patient was with the Geeveston crew for an hour before assistance arrived by road crew, and 20 minutes post this was retrieved with the chopper. He was commenced on NIV but deteriorated further and was intubated in ED and sent to ICU.
This patient survived and is now living back down in Geeveston; however, he has not made any further contact with the local GP services.
Paul provided details for the staff of the patients journey once leaving them, events in ED and a basic over view of his stay in the Royal.
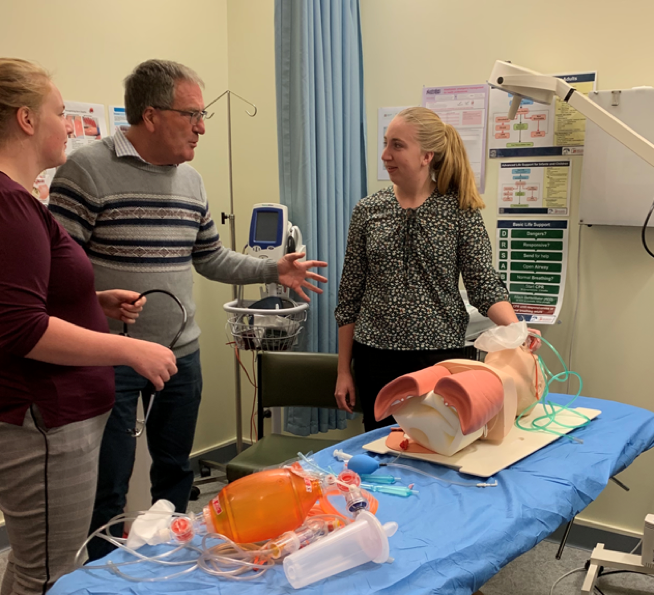
The discussion of this case tied in nicely and allowed an opportunity to answer a lot of question from the GP’s regarding packaging patients for retrieval and obtaining a PEEP valve for their BVM.
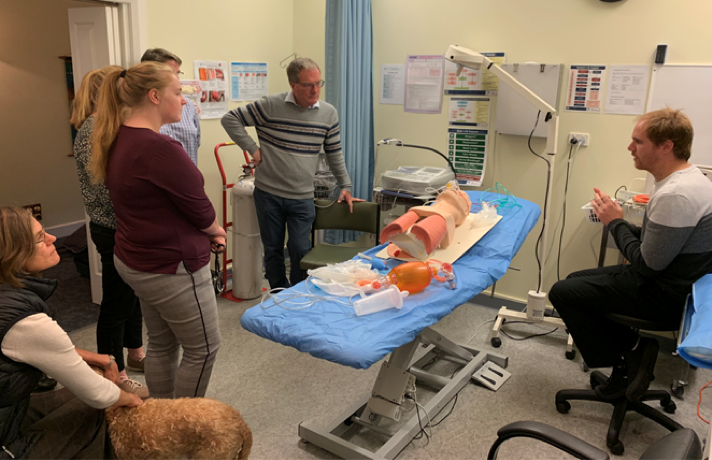
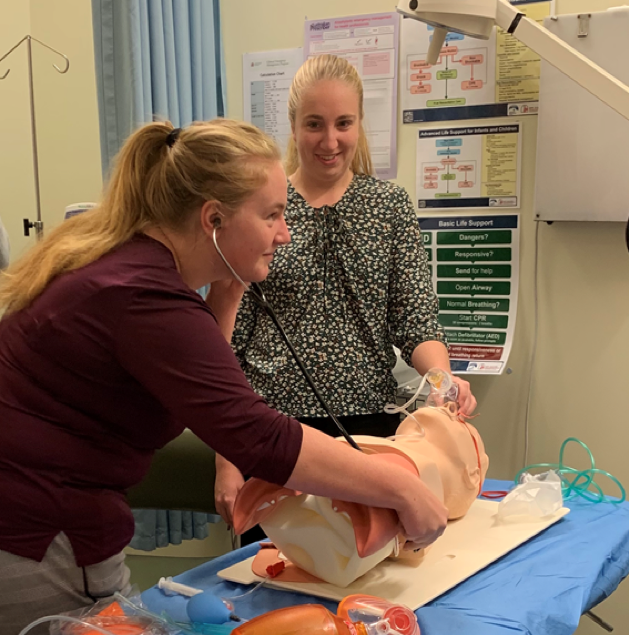
After talking through the case Paul led a scenario of an asthmatic self presenting to the clinic in moderate respiratory distress. This was great as each medical centre currently had a third year med student with them so it forced them to get involved and also meant the GP’s helped run the scenario – it was an all hands on deck approach and ran smoothly.
Next week Brian is off to Huonville to teach about point of care Ultrasound and also discuss any recent cases the staff want covered
| Sarah has been an RN for 14 years, 10 of those in the RHH ED. After several years on the floor it felt like the right time for some project work, and what better way to do it than by stalking her husband, Juan, professionally – once known as the ‘sepsis’ couple, the Ascencio-Lane’s have now taken over the EMET portfolio. When not in the office Sarah is either under pressure in the Hyperbaric Unit, or under even more pressure at home caring for their three young boys. |


 RSS Feed
RSS Feed
