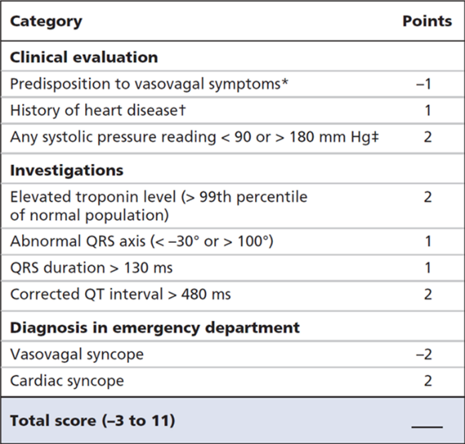
The risk score is mostly a quantification of what we evaluate already. History, ECG, ED diagnosis and troponin (if performed). Score ranges from -3 to 11 and patients are put into one of five categories; very low, low, medium, high or very high risk.
The primary outcome was “30-day serious outcomes” as determined during medical record review, telephone follow up, return visits, and coroners’ database.
Results?
The proportion of patients with serious outcomes increased from 0.3% in the very low risk group to 51% in the very high risk group.
This seems ok but I’m not so sure this “rule” will gain traction.
First, it’s too complicated to commit to memory. We would need to refer to MDCalc which will decrease its utility.
Second, it hasn’t formally been compared to what we already do… which is gestalt. (However, some may argue that it is already heavily reliant on gestalt.) It is possible that following the rule could make things worse.
Third, we know rules tend to perform less well in complex disease processes. This is why doctors have not been replaced by robots… yet.
How might I use the rule?
Probably how we use most rules; something we can write in the medical record to support a decision we have already made. This might sound cynical, but gestalt is probably the best rule.
Covering:
Thiruganasambandamoorthy V, Sivilotti M, Le Sage N, et al. Multicenter Emergency Department Validation of the Canadian Syncope Risk Score. JAMA Intern Med. 2020;180:737-44. [link to article]
| Dr Brian Doyle is an emergency physician originally from the United States but now very much calls Tasmania his home. Unfortunately, it will now be a bit more difficult to deport him from the country as he passed his Australian citizenship test a few years ago. (He was able to answer that Phar Lap won the Melbourne rather than the Davis Cup). His main interests are mostly the clinical aspects of emergency medicine but also in education, ultrasound and critical appraisal of the literature. He spends much of his time annoying people to help out with conferences. |


 RSS Feed
RSS Feed
